Lethal Injection
Compounding Pharmacies
COMPOUNDING PHARMACIES AND LETHAL INJECTION
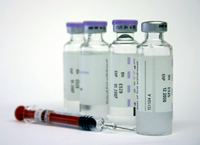
As drug shortages and actions by pharmaceutical manufacturers have
made it more difficult for prisons to obtain the drugs used in lethal
injections, some states have turned to compounding pharmacies as sources
of execution drugs. Compounding pharmacies do not face the same
approval process for their products that large manufacturers face,
leading to concerns about the safety and efficacy of their products.
What are compounding pharmacies?
Compounding pharmacies combine, mix, or alter drugs; traditionally compounding is used to meet the specific needs of an individual patient in response to a prescription. For example, a drug might be altered to remove an inactive ingredient for a patient with an allergy, or a medication that typically comes in pill form might be put into liquid form for a child who can’t swallow pills. However, some compounding pharmacies are more like drug manufacturers, producing large quantities of drugs that are copies or near-copies of commercially-available drugs, rather than customizing drugs for specific prescriptions. The Food and Drug Administration does not approve the products of compounding pharmacies. Compounding pharmacies must be licensed by their state’s pharmacy board, but do not have to register with the FDA or inform the FDA what drugs they are making.
On November 18, 2013, Congress passed the Drug Quality and Security Act. President Obama signed the bill into law on November 27th. The act allows large-scale compounding pharmacies to register as “outsourcing facilities,” which will be subject to FDA regulations. Compounders that do not register may still mix prescriptions for individual patients or produce limited quantities ahead of prescriptions without federal oversight. (New York Times, 11/18/13.)
Are compounding pharmacies accredited? Are their products safe?
Compounding pharmacies in the United States may be accredited by the Pharmacy Compounding Accreditation Board,
but accreditation is not required. The Board requires that accredited
pharmacies use high-quality chemicals and equipment, give pharmacists
and technicians regular training, test products for quality, and have an
effective recall mechanism in place. Only about 180 pharmacies in the
United States have received accreditation.

The International Academy of Compounding Pharmacists is an international organization based in Texas, consisting of over 2700 pharmacists and other members of the pharmacy community who focus on compounding. The IACP’s mission is “to protect, promote and advance the art and science of pharmacy compounding.”
In 2012, a compounding pharmacy in Massachusetts was found to be the source of an outbreak of fungal meningitis that infected over 700 people in 20 states, leaving 61 dead (New York Times, 10/26/12; Centers for Disease Control, 7/1/13). The New England Compounding Center was not accredited, and produced large quantities of drugs for hospitals across the country, rather than the traditional compounding practice of producing small quantities in response to individual needs. An FDA investigation found mold and bacteria in areas that should have been sterile and discovered microbial growth in all 50 tested vials of methylprednisolone acetate, an injectable pain medication that was linked to the meningitis outbreak. The New England Compounding Center voluntarily recalled all of its products, ceased operations, and handed its license over to the Massachusetts Board of Registration in Pharmacy in October, 2012 (FDA, 11/1/12).
Congress held hearings in response to the outbreak to determine what regulatory action might prevent future outbreaks. The CEO of IACP testified at the hearings and voiced support for increased oversight of compounding pharmacies that manufacture new drugs, rather than altering drugs for the use of individual patients. In May, 2013, a Senate committee approved a bill that would give the FDA greater authority over compounding pharmacies (New York Times, 5/22/13).
UPDATE: The CDC said that 63 people have died from the fungal meningitis outbreak linked to compounding pharmacies, including 24 people in 2013. The FDA has reported 14 multistate or national voluntary recalls of compounding pharmacy products in 2013. (Wall Street Journal, 9/9/13)
States’ use of lethal injection drugs from compounding pharmacies
(For a list of states that have used compounded drugs in executions or announced intentions to do so, visit our State-by-State Lethal Injection page.)
As lethal injection drugs have become less accessible due to a combination of shortages and measures implemented by pharmaceutical companies intended to stop the drugs’ use in executions, some Departments of Corrections have begun to use compounding pharmacies as a source of those drugs. South Dakota obtained pentobarbital, an anesthetic used in executions, from a compounding pharmacy for the October 15, 2012 execution of Eric Robert. The same source was likely used in the October 30, 2012 execution of Donald Moeller, but the Department of Corrections did not release information on the drug (Reprieve, 6/18/13).
In 2012, in response to a court order to reveal the source of its lethal injection drugs, Pennsylvania announced that the drugs were obtained from compounding pharmacies (Patriot-News, 11/6/12). Pennsylvania’s execution protocol is the subject of a federal class action lawsuit. No executions have been carried out in the state since 1999. In March 2013, in anticipation of an execution that was later stayed on unrelated grounds, the Director of Colorado’s Department of Corrections wrote a letter to 97 compounding pharmacies in the state, asking them to provide sodium thiopental for the execution (The Denver Post, 3/12/13).
After Georgia’s supply of pentobarbital expired in March 2013, the state announced that it planned to obtain a new supply from a compounding pharmacy for the scheduled execution of Warren Hill (Associated Press, 7/11/13). Hill’s execution was carried out in 2015.
In 2018, investigative reporter Chris McDaniel discovered that Texas secretly obtained execution drugs from the Greenpark Compounding Pharmacy, a pharmacy that the Texas State Board of Pharmacy has cited for 48 violations in the past eight years, including “keeping out-of-date drugs in stock, using improper procedures to prepare IV solutions, and inadequate cleaning of hands and gloves.” Greenpark’s license was put on probation in November 2016 after it botched a prescription for three children, sending one of them to the hospital for emergency care. (BuzzFeed News 11/28/18)
More Information
- Chris McDaniel, “Inmates Said The Drug Burned As They Died. This Is How Texas Gets Its Execution Drugs,” BuzzFeed News, November 28, 2018.
- Forbes: “Why Don’t Pharmacy Groups Condemn Lethal Injection Role?” (5/14/2014)
- Austin American-Statesman: “Commentary: Compounding Pharmacies Benefit Texans” (Op-ed by four compounding pharmacists, 7/29/14)

